Why Choosing the Right Ventilator Machine is Crucial for Care?
In the ever-evolving healthcare landscape, the importance of selecting the right Ventilator Machine cannot be overstated. A definitive report from the World Health Organization reveals that approximately 15% of patients requiring intensive care are ventilated. This statistic highlights the pivotal role these machines play in critical care settings. The right ventilator can significantly improve patient outcomes, but making the wrong choice can lead to dire consequences.
Dr. Emily Chen, a renowned expert in respiratory therapy, once stated, "The efficiency of a Ventilator Machine directly correlates with patient survival rates." This underscores the importance of understanding machine capabilities and patient needs. Each ventilator is designed with unique settings and functions, necessitating thorough knowledge before selection. Inadequate choices can stem from various pressures, including time constraints and a lack of training.
Moreover, it’s vital to reflect on the inherent complexities associated with Ventilator Machines. While many hospitals have advanced technology, not all staff are adequately trained to operate these machines effectively. Patient demographics, underlying conditions, and ventilation strategies must all be considered. Failure to recognize these factors can compromise care quality and patient safety. Thus, careful deliberation in choosing a Ventilator Machine isn’t just critical—it’s essential for effective patient management.
Understanding the Role of Ventilator Machines in Patient Care
Ventilator machines play a vital role in patient care, especially in critical settings. These devices support breathing and ensure adequate oxygenation. According to the World Health Organization, millions of patients worldwide require mechanical ventilation each year due to respiratory failure. The choice of ventilator can significantly influence patient outcomes, highlighting the importance of selecting the right machine.
Different models come with unique features like modes of ventilation and monitoring capabilities. Research shows that using advanced ventilators can reduce the risk of ventilator-associated pneumonia by 30%. However, it’s crucial to understand that not every patient benefits from high-tech options. Some may require simpler machines tailored to their specific needs. This highlights the importance of individual assessment before machine selection.
Tip: Regular training for healthcare professionals on ventilator usage is essential. Knowledge gaps can lead to inappropriate settings or misunderstandings about patient needs. Keep a checklist of common ventilator settings for various conditions handy. Another tip: routinely evaluate patient responses to ventilation. The goal is not just to use technology but to ensure it aligns with improving patient care. Continuous monitoring is key, as techniques and patient conditions can change rapidly.
Importance of Different Ventilator Modes in Patient Care
This chart illustrates the usage percentage of different ventilator modes in patient care. Understanding which modes are utilized most frequently can help healthcare providers select the appropriate ventilator settings for optimal patient outcomes.
Factors to Consider When Selecting a Ventilator Machine
Choosing the right ventilator machine is vital in patient care. Various factors play a crucial role in this process. First, the patient's specific needs guide the selection. Some patients require invasive support, while others may respond better to non-invasive methods. Understanding these nuances is essential for effective treatment.
Next, airflow capabilities are important. A machine must deliver adequate volumes and pressures for each patient. If the ventilator cannot meet these needs, patients may face serious risks. Additionally, consider the interface options. Choosing the right mask or tube can significantly affect comfort and compliance.
Lastly, reliability in monitoring is key. A ventilator should provide accurate readings of vital parameters. Subpar monitoring can lead to missed warning signs. Training staff on the device is also crucial. Even the best machine may be inadequately used without proper understanding. Each of these elements contributes to better patient outcomes.
Types of Ventilator Machines and Their Specific Applications
Choosing the right ventilator machine is essential for effective patient care. There are various types of ventilators, each suited for specific medical situations. Invasive ventilators are often used for patients requiring respiratory support in intensive care units. According to a market report by the Global Ventilator Market, these machines account for a significant portion of the market due to their complexity and effectiveness in critical care.
Non-invasive ventilators, such as BiPAP and CPAP, are designed for patients with respiratory issues that do not require intubation. Studies have shown that these machines can reduce the risk of complications associated with invasive methods. They are beneficial for treating conditions like chronic obstructive pulmonary disease (COPD) and sleep apnea. Their ease of use is vital, promoting patient comfort and compliance.
However, selecting a ventilator isn’t straightforward. Factors like patient age, weight, and specific respiratory conditions play a role. A mismatch can lead to inadequate ventilation or patient discomfort. Data indicates that up to 30% of patients may experience complications due to incorrect ventilator settings. This highlights the need for careful selection and monitoring by trained healthcare professionals.
Why Choosing the Right Ventilator Machine is Crucial for Care? - Types of Ventilator Machines and Their Specific Applications
| Type of Ventilator | Description | Specific Applications |
|---|---|---|
| Invasive Ventilator | Delivers airflow through an endotracheal tube. | Severe respiratory failure, Intensive Care Units (ICUs). |
| Non-Invasive Ventilator | Delivers airflow through a facial or nasal mask. | Chronic obstructive pulmonary disease (COPD), Sleep apnea. |
| Portable Ventilator | Lightweight, easy to transport, often battery-operated. | Emergency situations, home care. |
| Pediatric Ventilator | Specifically designed for infants and children. | Respiratory support in neonatology and pediatrics. |
| Bi-Level Positive Airway Pressure (BiPAP) | Offers different pressure levels for inhalation and exhalation. | Pulmonary edema, restrictive lung disease. |
The Impact of Ventilator Choice on Patient Outcomes
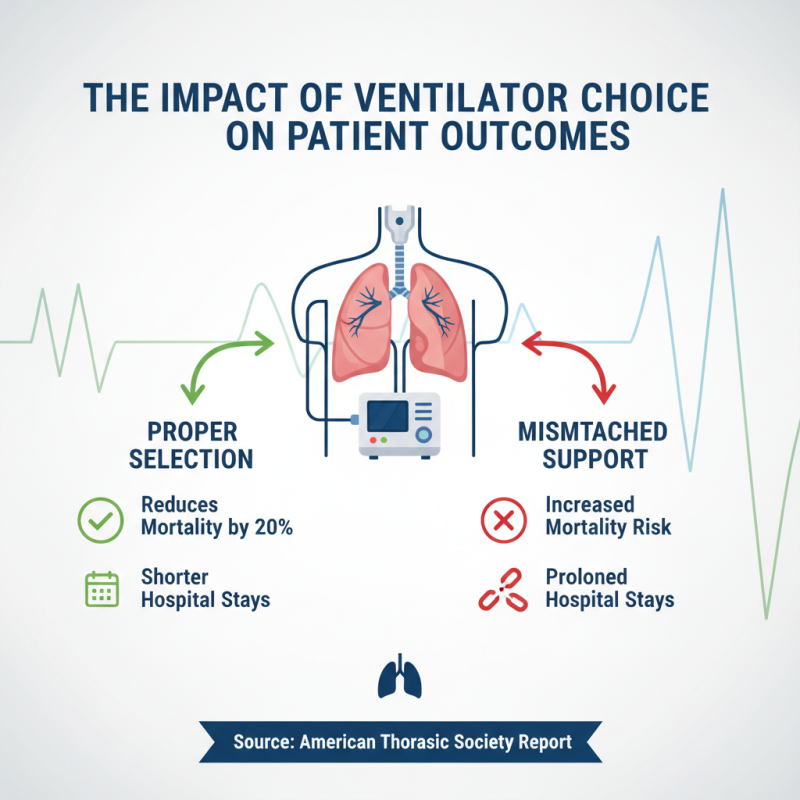
The choice of ventilator can significantly impact patient outcomes. Studies indicate that the proper selection of a ventilator can reduce mortality rates in critically ill patients by as much as 20%. A report by the American Thoracic Society highlights that mismatched ventilatory support often leads to prolonged hospital stays and worsened respiratory conditions.
Different machines offer varied functionalities. For example, some ventilators provide high-frequency oscillation that benefits patients with severe acute respiratory distress syndrome (ARDS). Data shows that ventilators with adaptive settings may improve oxygenation and minimize lung injury. Yet, not all healthcare providers have access to advanced models. This discrepancy raises questions about equitable care and the potential for adverse outcomes.
Patient-ventilator synchrony is also crucial. Many machines fail to adapt seamlessly to patients' needs. The result? Increased work of breathing and discomfort for the patient. The literature illustrates that improper ventilator adjustments can lead to lung over-distension. Ongoing training and awareness of ventilator technology should be prioritized. This ensures that healthcare providers can make informed decisions that directly influence patient recovery trajectories.
Common Challenges in Ventilator Selection and Usage
Choosing the right ventilator machine involves navigating various challenges. A report by the American Association for Respiratory Care noted that improper ventilator selection can lead to increased morbidity rates. The complexity of patient needs requires careful consideration. Factors such as lung mechanics, breathing pattern, and disease severity must be evaluated.
A common issue is the learning curve for healthcare providers. Many professionals feel unprepared to operate advanced ventilators. According to a survey, nearly 70% of clinicians reported inadequate training on ventilator management. This highlights the need for continuous education. Familiarity with the equipment is critical for effective patient care.
Tips:
1. Ensure ongoing training sessions for staff.
2. Evaluate ventilator features regularly to align with patient needs.
3. Encourage a culture of asking questions and seeking help.
Reflections are essential. Ventilator strategies that work in one scenario may not apply in another. It's crucial to be adaptable. Continuous assessment can improve outcomes, but it requires a commitment to learning and self-evaluation.
Related Posts
-

What is a Mining Lamp Charger and How Does It Work?
-

How to Enhance Indoor Air Quality with Advanced Ventilation Machines for Healthier Living Spaces
-

Top 5 Mining Jack Hammers for Efficient Rock Breaking and Drilling
-

What is Mining Lamp Charger Trends at 2026 Canton Fair?
-

Exploring the Benefits of Portable Ventilators: Your Guide to Respiratory Relief Anytime, Anywhere
-

Top Pneumatic Equipment Types You Should Know About?



